医科学専攻
- Master's Courses
修士課程 - Doctoral Courses
博士課程
Renal and Circulatory Therapeutic Innovation腎・循環治療創成学(医工研究科)
STAFF
Professor
-
Toyohara, TakafumiProfessor.M.D. Ph.D. 豊原 敬文 教授 (兼任)

CONTACT
TEL:+81-22-717-7163
E-MAIL:takafumi.toyohara.e6*tohoku.ac.jp
(「*」を「@」に変換してください)
OUTLINE
Overview:
Our division focuses on the kidney and the circulatory system, which are central to whole-body homeostasis. By integrating medicine, engineering, and data science, we aim to implement systemic resilience (resistance to and recovery from disease), rejuvenation, and regeneration. Specifically, the kidney regulates fluid volume, electrolytes, metabolites, and toxins, while the circulatory system controls blood pressure and blood flow and transports and clears humoral factors—such as hormones, cytokines, and metabolites—to coordinate inter-organ crosstalk. To address fundamental unmet needs and questions arising from clinical practice, we develop iPSC-based disease models (disease-in-a-dish) and engineered human organ models, and use these platforms to elucidate disease mechanisms and evaluate therapeutic candidates. We further pursue bidirectional translational research—from bedside to bench and back to bedside—to develop new therapies and deliver them to patients.
Research themes:
• Mechanisms of vascular and renal aging, inter-organ crosstalk, and Ageotype analyses
• Strategies to enhance systemic resilience, promote rejuvenation, and develop regenerative therapies
• Organelle (e.g., mitochondrial) dysfunction in disease and therapeutic development
• Engineering iPSC-based human organ models and their applications
本研究分野は、全身恒常性を担う腎臓と循環系に着目し、医学・工学・データ科学を融合して、全身レジリエンス(病態への抵抗性・回復力)の向上、若返り、再生の実装を目指します。具体的には、腎臓は体液量・電解質・代謝物・毒素を調節し、循環系は血圧・血流を制御するとともに、ホルモン・サイトカイン・代謝物などの液性因子を搬送・回収して臓器連関を成立させます。臨床現場での根本的な課題や疑問についてiPS細胞を用いた疾患モデル(disease-in-a-dish)や工学的ヒト臓器モデルを構築し、機序の解明と治療候補の検証を進めていきます。さらにbedside to bench, bench to bedsideの橋渡し研究を実践し、新たな治療を開発します。
研究テーマ:
• 血管や腎臓の老化メカニズムや全身臓器との連関、Ageotypeの解析
• 全身臓器のレジリエンス向上・若返り、再生治療の開発
• ミトコンドリアなどの細胞内小器官と病態との関連解析、治療法開発
• iPS細胞などを用いた工学的ヒト臓器モデルの構築
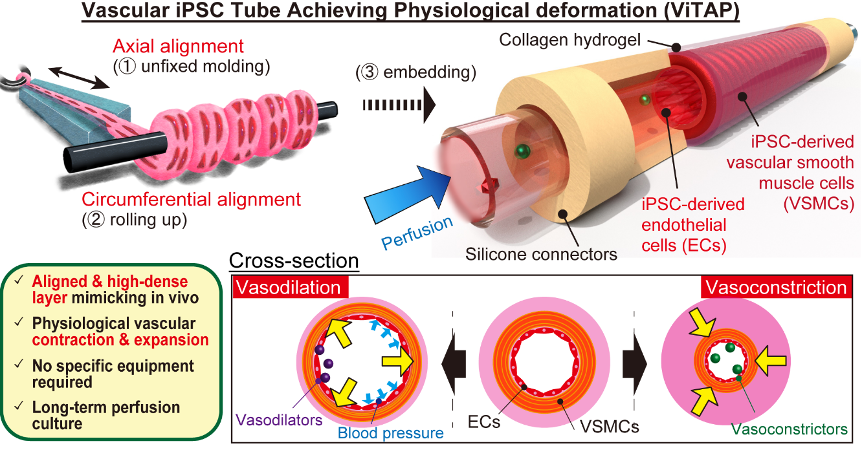
Engineered human vascular graft model
工学的ヒト人工血管モデル
3D bioprinting–based fabrication of blood vessels
バイオ3Dプリンターによる血管作製
ARTICLE
Uramoto S, et al. Three-dimensional intestinal tube with a crypt-like uneven inner wall fabricated using electrolysis-generated microbubbles Lab Chip 26: 541, 2026.
Watanabe S, et al. LUBI-CKD TRIAL Investigators. Lubiprostone in chronic kidney disease: Insights into mitochondrial function and polyamines from a randomized phase 2 clinical trial. Sci. Adv. 29: eadw3934. 2025.
Tongu Y, et al. Mitochondria-homing drug mitochonic acid 5 improves Barth syndrome myopathy in a human-induced pluripotent stem cell model and Barth syndrome drosophila model. FASEB J. 39: e70739, 2025
Oshita T, et al. Urinary growth differentiation factor 15 predicts renal function decline in diabetic kidney disease. Sci. Rep. 13:12508, 2023.
Toyohara T, et al. Patient hiPSCs Identify Vascular Smooth Muscle Arylacetamide Deacetylase as Protective against Atherosclerosis. Cell Stem Cell 27: 147-157, 2020.
